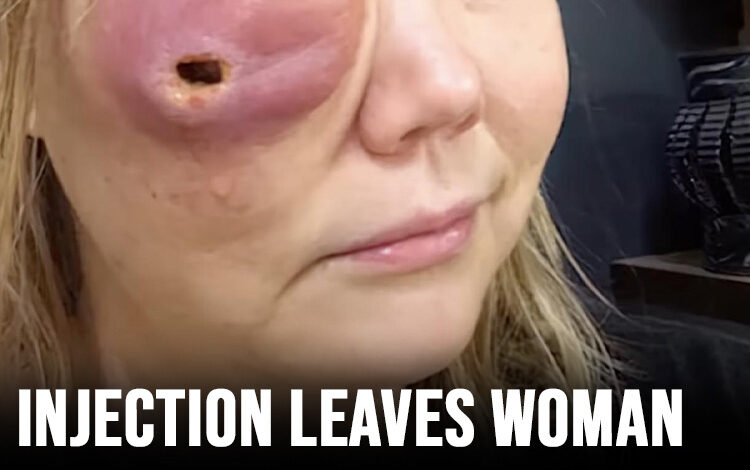
Gina Anderson was left with a big hole in her face after filler failure – this is her today, 6 years later
In an era where facial refinement—from lip augmentations to forehead smoothing—has moved from the fringes of Hollywood to the mainstream of suburbia, the barrier to entry has never been lower. The marketplace is saturated with “specialists” promising eternal youth at competitive prices. Yet, as the industry swells, the line between medical excellence and dangerous opportunism continues to blur.
For most, the stakes are aesthetic. For Gina Anderson, a neurologist based in Oregon, the stakes became a fight for her own anatomy. It is a cautionary tale that highlights a chilling irony: even those with medical degrees can fall victim to the “quick fix” culture when the practitioner across the needle isn’t who they claim to be.

The 40th Birthday Decision
The catalyst was a common milestone. Upon turning 40, Anderson felt the familiar pressure to “freshen up” her appearance. When a colleague offered to administer cosmetic fillers, the convenience outweighed the caution.
“A colleague offered to do fillers for me, and it was like, ‘Well, I’m in my 40s, I’m going to look a little bit better,’” Anderson shared during an appearance on the reality medical series Botched.
Operating under the assumption that she was receiving FDA-approved hyaluronic acid treatments like Restylane or Juvederm, Anderson moved forward. She didn’t realize until years later that the substance entering her tissue wasn’t a temporary filler, but permanent, medical-grade silicone—an illegal and dangerous substitute in this context.
From Inflammation to “The Boom”
The biological fallout was not immediate, but it was devastating. While Anderson had injections in both cheeks, the left side remained largely unaffected. Her right side, however, became the site of a localized war. The silicone triggered a massive inflammatory response, resulting in a granuloma.
Note: According to the Mayo Clinic, a granuloma is a defensive cluster of immune cells that form when the body attempts to wall off foreign substances or infections it cannot eliminate.
For four years, the silicone sat like a ticking time bomb. When it finally reached a breaking point, the transformation was hauntingly rapid. Anderson describes a sudden, violent escalation where the skin could no longer contain the internal pressure.
“All of a sudden, it just went boom,” Anderson recalled. The resulting rupture left her with a gaping hole in her cheek and a severely deformed eye area. Her face, quite literally, began to fall apart.

The Reality of Reconstruction
The journey to reclaim her face eventually led Anderson to the surgical suites of Botched, where specialists work to undo the damage caused by “back-alley” or negligent cosmetic procedures. Her case serves as a stark reminder of the “Self-Acceptance vs. Alteration” dichotomy.
While the freedom to modify one’s appearance—whether through fitness, fashion, or surgery—is a personal right, the medical community warns that research is the only true safety net. ### Expert Advice for Prospective Patients If you are considering a cosmetic procedure, keep the following in mind to avoid a similar tragedy:
- Verify Credentials: Ensure your provider is a board-certified plastic surgeon or dermatologist.
- Know the Product: Always ask to see the vial and the packaging of the filler being used.
- Beware “Deals”: If the price seems too good to be true, the product may be an illegal or industrial-grade substitute.
Gina Anderson’s experience is a sobering testament to the fact that your body is not a canvas for shortcuts. True self-confidence comes from being comfortable in your own skin, but if you choose to change it, ensure the hands holding the scalpel—or the syringe—are legitimate.
When the biological ticking time bomb finally detonated in Gina Anderson’s face, the fallout was more than aesthetic—it was systemic. For Anderson, an Oregon-based neurologist, the illegal silicone injections she had received years prior led to a catastrophic physical and professional collapse. After five failed corrective surgeries, she was left not only with a gaping hole in her cheek but with a life that had become unrecognizable.
The toll was so severe that Anderson was forced to shutter her medical practice. “You can’t sleep, and you’re in constant pain,” she revealed. “It’s hard to think on your feet all the time.” The crisis extended beyond the localized inflammation; she reported chronic agony, fatigue, and even telogen effluvium—a form of hair loss triggered by the immense stress on her body. “It’s been a nightmare,” she stated, describing a state of constant exhaustion and diminished cognitive function.

A “Smoldering” Inflammatory Response
Desperate for a definitive solution, Anderson sought the expertise of Dr. Terry Dubrow and Dr. Paul Nassif on the medical series Botched. Dr. Dubrow noted a disturbing anomaly in her case: while granulomas (foreign body inflammatory reactions) typically surface within six months to a year, Anderson’s didn’t manifest until much later.
“The fact that Gina didn’t start developing those granulomas until way later indicates it’s a very slow, smoldering inflammatory chronic response,” Dubrow explained, noting that such delayed reactions can be “impossible to treat.”

Inside the Operating Room
Dr. Nassif took the lead on the reconstructive effort, which involved complex procedures to clear the debris left by previous failed attempts and the original silicone. During the initial surgery, Nassif made a startling discovery: he removed a foreign object from her facial tissue that appeared to be a “piece of gauze” left behind from a prior operation.
To restore the destroyed contours of her face, the surgeons performed a fat transfer, harvesting tissue from her abdomen to provide necessary volume to her cheek. For a brief window, it seemed the “personal hell” had ended—Anderson’s pain subsided, and she was finally able to sleep.
The Complication: Recurrent Seromas
The relief, however, was short-lived. In a stark illustration of the unpredictability of “silicone-damaged” tissue, Anderson developed recurrent seromas—persistent pockets of fluid that caused her cheek to swell once more.
“Gina’s body is constantly making fluid in her cheek… why is this happening? I don’t know,” Dr. Nassif admitted, highlighting the volatile nature of healing after illicit cosmetic injections. The only recourse was a second intensive surgery to locate and remove the seroma capsule.

The Turning Point
The second procedure proved to be the “miracle” Anderson had been searching for. Following the final intervention, the transformation was not just visible in her reflection, but in her overall vitality.
The signs of recovery included:
- Cognitive Clarity: Anderson reported her “thought process is actually getting faster.”
- Physical Health: Her hair loss ceased and began to regrow.
- Emotional Stability: An increase in energy levels and a significantly improved mood.
“It’s just life-changing,” Anderson said of the results. Today, she appears rejuvenated, with her facial symmetry largely restored and her health returning to its baseline.

A Final Warning
The saga of Gina Anderson serves as a powerful reminder of the risks inherent in the cosmetic industry. While the desire for self-improvement is a personal journey, the medical community maintains a rigid stance: Plastic surgery should only be performed by board-certified specialists. Beyond the technical risks, there is the psychological component of self-image. While we may strive to alter parts of our appearance, the ultimate goal remains finding confidence and value in who we are. In the end, your health and your identity are your most precious assets—protect them with due diligence.